Table of Contents
ToggleWhat is ringworm?
Ringworm in dogs is a fungal infection of the skin, despite the slightly confusing name (it’s not actually a worm). It can be caused by more than 30 species of a group of fungi called dermatophytes, giving ringworm’s clinical name of dermatophytosis (1).
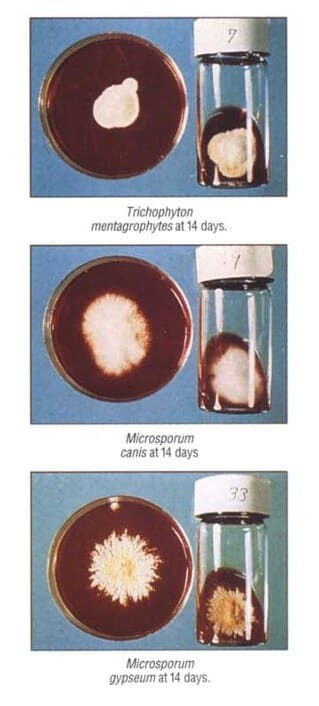
The most common species that affects dogs is Microsporum canis. This dermatophyte is specially adapted to living on a host.
Another species, Microsporum gypseum, normally lives in the soil and feeds off decomposing keratin in hair. Sometimes, M. gypseum can infect dogs after they have close contact with contaminated soil. The other common dermatophyte that causes ringworm in dogs is Trichophyton mentagrophytes, which normally infects rodents, rabbits, and hedgehogs but can also infect dogs but is more common in cats, who hunt and are more likely to encounter infected rodents (1).
Ringworm is a zoonotic disease, which means it can be passed from an infected animal to a person. If your dog has ringworm, you will have to take extra care to make sure that you don’t get a skin infection as well. Ringworm is treatable and not life-threatening, but it can be uncomfortable.
How do dogs get ringworm?
Ringworm is a contagious disease. The most common way to get ringworm in dogs is through direct contact with another infected animal.
Dogs can also become infected from contact with spores in the environment, but this method of spread requires the spore to be deposited into a small skin wound, known as a microtrauma. This could be caused by a number of factors, including grooming appliances such as clippers, which can cause microscopic skin wounds that are invisible to the naked eye but large enough to allow a dermatophyte spore to start an infection (1, 2). Equally, the presence of high humidity, skin parasites, and other causes of itching can contribute to an increased risk of environmental dermatophyte spores gaining a foothold in the skin.
Once the spores have been transferred to a new dog, they begin to hatch and form fungal structures that invade the outer layer of the skin. The symptoms of ringworm, in the form of skin lesions, appear between one and three weeks after infection (1).
Ringworm symptoms in dogs
Ringworm in dogs can be tricky to spot, and the symptoms are varied. The symptoms are produced by a combination of the fungal structures invading the skin and the production of enzymes that digest keratin, an important structural protein in hair and skin (1).
Most commonly, ringworm in dogs looks like circular patches of skin that develop scales or dandruff with hair loss (alopecia). The remaining hairs at the edge of the area are brittle and very prone to breaking. The skin might be red and can be itchy. As the lesion develops, brown crusts of dried secretion can form alongside small, red, raised areas of skin (papules). If the skin is very itchy, these lesions will be complicated by the dog scratching itself and causing self-trauma.
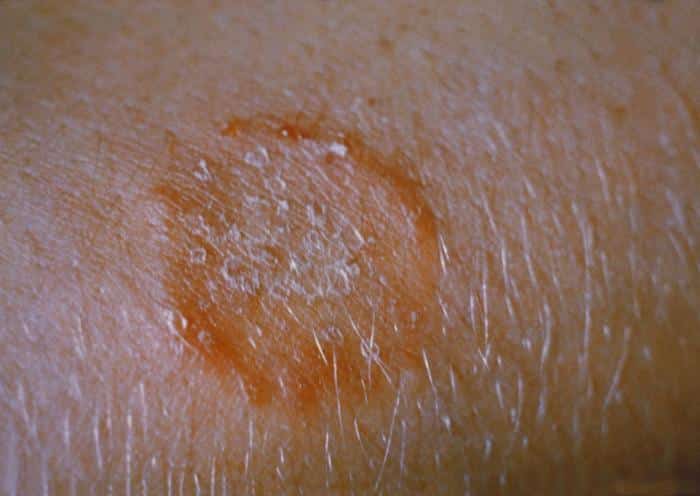
The initial lesions will occur where the dog was first infected. Since dogs like to explore with their noses, the face, ears, head, and paws are some of the most common areas. As the first lesion develops, ringworm can spread to other areas of the body, causing patchy areas of hair loss and scaling (3).
There are less common patterns of skin lesions, such as a kerion reaction, which presents as a single or multiple, raised, dome-shaped nodules.
Another uncommon pattern is the formation of pseudomycetomas or mycetomas, which appear as nodules that ulcerate and drain pus before forming chronic, non-healing wounds (2).
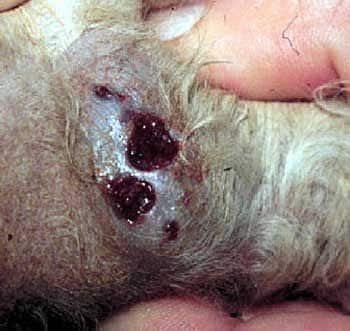
Ringworm can also affect the nails, although this presentation without skin lesions is uncommon. The affected nail might be easily damaged, discoloured, and malformed (4).
Overall, ringworm in dogs can produce a variety of different lesions, and any area of scaling and hair loss, regardless of the shape or itchiness, could be suspicious of ringworm.
How is ringworm diagnosed?
Given that ringworm in dogs can be difficult to recognise from the symptoms alone your vet might recommend some extra diagnostic tests to confirm or exclude the diagnosis. Even with testing, dermatophytes can be tricky to identify as they take a long time to grow in the laboratory. You might have to try a combination of tests before getting a definitive answer.
Wood’s Lamp
The simplest test is an examination with a Wood’s lamp, an ultraviolet lamp invented by Robert Wood in 1903. If the skin lesions fluoresce green under Wood’s lamp, then they are caused by a dermatophyte. However, a negative result does not exclude ringworm as a diagnosis. Between 26 and 70% of M. canis and any M. gypseum or Trichophyton infections don’t fluoresce and so won’t be detected by the Wood’s lamp (1, 2).

Microscopy
The next step is to take samples of hair and superficial skin for analysis under the microscope or for fungal culture. Looking for fungal structures under the microscope can give an indication of whether fungi are present. However, this can also give false negative results, so a follow-up culture is usually recommended.

Fungal Culture
If fungal structures are seen under the microscope, it’s usually best to complement the initial diagnosis with a culture to identify the species of fungus that was seen (2). Fungal culture itself can be tricky. The results usually take two weeks to come back from an external laboratory, so your vet might suggest starting treatment before a positive confirmation of the diagnosis.
Some vets use an in clinic fungal culture called Fungassay, which may detect early positive ringworm results from 7-14 days. Samples of hair or scale from suspicious lesions are used to inoculate the culture. Evaluation of the test medium can begin as early as 48 hours post inoculation.
PCR Testing
A faster method of diagnosis is to look for fungal DNA using a PCR test. This test is very sensitive and will detect DNA from dead dermatophytes, so it’s best used as an initial diagnostic test rather than for monitoring treatment. While it’s much faster, a PCR test might be more expensive, so discuss with your vet what diagnostic options are available (2).
Skin Biopsy
For cases with an unusual presentation, such as the kerion reaction, or chronic, non-healing wounds, your vet might recommend taking a skin biopsy. This can be a good diagnostic tool for tricky cases and is likely to give a quality answer. The biopsy will be sent to a pathologist, who can use stains to make the fungal structures easier to visualise (2).
Ringworm treatment for dogs
Ringworm treatment can be split into three categories: topical treatment, systemic treatment, and environmental decontamination. How to get rid of ringworm in your particular puppy’s case will depend on the number and location of the lesions, as well as the severity of the infection. Always consult your veterinarian to formulate a tailored plan for how to treat ringworm in dogs at home.
Topical treatment
The aim of topical treatment is to decrease the number of dermatophytes present on the dog’s hair and skin, as well as the chance of transmission to other dogs and people.
Shampoos
The most common topical treatment is a twice-weekly bath using a shampoo for ringworm in dogs that contains anti-fungal medications like enilconazole, econazole or miconazole combined with the disinfectant chlorhexidine. Examples of this type of product are Malaseb or Sebazole Shampoo.
Creams
For lesions on difficult to wash areas, such as the head and ears, a miconazole cream, such as Ilium Fungafite, can be just as effective (2).
Natural Home Remedies
Prefer to treat ringworm in dogs naturally at home? In our experience ringworm home remedies are generally only beneficial in the mildest of cases, such as a single localised lesion.

Trimming the hair in affected areas is not always necessary and can increase the risk of the ringworm spreading.
Systemic treatment
Systemic treatment aims to target the fungus in places where the topical treatment can’t reach, such as the hair follicles. In healthy animals, ringworm infection is usually self-limiting, but systemic treatment can reduce the time needed for the infection to resolve.
The most common systemic treatments for ringworm in dogs are itraconazole, ketaconazole, fluconazole, and terbinafine, which are available as tablets. There are a variety of treatment protocols. Most experts recommend continuing treatments until the fungus can no longer be detected using diagnostic tests, which can take between four and eight weeks (1, 2).
Environmental decontamination
Environmental decontamination is an important part of any treatment regimen. Removing dermatophyte spores from the environment will reduce the risk of transmitting the disease to other animals and people.
Additionally, if you’re using fungal culture or PCR as a benchmark for when to stop treatment, removing as much fungal material from the environment as possible will reduce the time of treatment.
All surfaces should be cleaned. First, they need to be swept or vacuumed to remove debris such as hair and mud. Then a disinfectant with good antifungal properties can be used to treat the area and reduce the number of spores. Over-the-counter cleaners with labels indicating an antifungal action are usually effective but need to be left on the surface for 10 minutes to give them time to work (1).
You might consider confining the affected dog to just one room in your house while the treatment is ongoing. This can be an effective way of limiting the amount of cleaning you have to do. You might want to limit the contact that vulnerable people, such as children or the elderly, have with your dog to reduce the risk of infection with ringworm.
How can you prevent ringworm in dogs?
Preventing ringworm can be tricky. There are no standard, regular treatments for prevention like there are for fleas, and there are no vaccines either. Since ringworm is mainly spread by direct contact with other infected animals, keeping your dog’s contact with high-risk pets to a minimum is one measure.
For example, if your dog goes to the groomer, they should have measures in place there to limit the chance of ringworm spreading, such as regularly clearing trimmed hair and cleaning clippers between pets.
Some ringworm infections result from dogs digging holes and other normal behaviours. It can be difficult to discourage dogs from engaging in these activities, and you might not want to either, since the risk is minimal.
Overall, you should be aware of the symptoms of ringworm in dogs so that if your pet does get an infection, you can act quickly before the infection spreads or gets worse.
FAQ
The most frequent questions and answers about ringworm in dogs.
Yes, dogs can get a fungal infection called ringworm. They usually contract it from other affected dogs but some types of fungus in the soil can infect dogs as well.
With effective treatment, ringworm can be eliminated from a dog’s skin in between four to eight weeks.
Ringworm will be contagious until it has been eliminated from your dog’s skin. This might require up to eight weeks of treatment. Fungal spores shed into the environment can survive for up to 18 months, but infection from spores is less common than via direct contact. Regular cleaning and disinfection during treatment will help to reduce the number of infective fungal particles in the environment.
Yes, ringworm can be passed from dogs to humans. The most common way of transmitting ringworm is by direct contact. Children under 5 years old, the elderly and immunocompromised people are at greater risk of being infected with ringworm. However, the infection is usually mild and can be treated.
Yes, dogs can get ringworm lesions on any part of their skin. The most common place to find lesions is on the head, face, ears and paws. Once an infection has started, it can spread to any other part of the dog’s skin.
Yes, cats can also be infected by ringworm and can act as a source of infection for dogs.
Despite the name, ringworm is not a worm at all. Ringworm is a fungus that affects the skin. If you’re noticing that your dog is passing worms in its poo then you should consult your vet.
References
- Moriello KA, Coyner K, Paterson S, Mignon B. Diagnosis and treatment of dermatophytosis in dogs and cats.: Clinical Consensus Guidelines of the World Association for Veterinary Dermatology. Vet Dermatol. 2017;28(3):266–8.
- Moriello K. Dermatophytosis in cats and dogs: A practical guide to diagnosis and treatment. In Pract. 2019;41(4):138–47.
- Paterson S. Dermatophytosis: an update. Companion Anim. 2017;22(5):248–53.
- Shaw SC. Dermatophytosis in dogs. Companion Anim. 2010;15(7):60–6.
- Joel Mills, CC BY-SA 3.0, via Wikimedia Commons
- Fungassay Dematophyte Test Medium by Zoetis
- Seawind60, CC BY-SA 4.0, via Wikimedia Commons
- Rjgalindo from es, CC BY-SA 3.0, via Wikimedia Commons
- self, CC BY-SA 3.0, via Wikimedia Commons



